We’ve already mentioned Telehealth in the context of digital healthcare, but this topic is very broad, so we want to cover it more in depth. Believe us it’s worth knowing about its possibilities as soon it might become a “must-have” tool for healthcare institutions all around the world.
Why so? Because the main purpose of Telehealth is to overcome any kind of barriers and provide equal access to medical care and services for patients in any part of the world, even in space. Telehealth also helps to get over those barriers especially when in-person therapy is impossible because of many problems such as scheduling, adverse weather, illness, and others. Or the pandemic.
Telehealth from the beginning

So what is Telehealth? Telehealth is a collection of means or methods for enhancing health care, public health, and health education delivery and support using telecommunications technologies.
Telehealth encompasses a broad variety of technologies and tactics to deliver virtual medical, health, and education services. It uses different forms of technology like email, smartphones, video calls, wireless, and many other communication types.
Telehealth is not a specific service, but a collection of solutions to enhance medical care and non-clinical services, such as provider training, administrative meetings, and continuing medical education, in addition to clinical services.
Information and communication technologies are the main drivers for Telehealth that have great potential to address some challenges faced by both developed and developing countries in providing accessible, cost-effective, high-quality health care services. Telemedicine uses tech innovations to overcome geographical barriers and increase access to health care services. This is particularly beneficial for rural and underserved communities in developing countries — groups that traditionally suffer from a lack of access to health care.
According to the Centers for Disease Control and Prevention, 15 percent of the U.S. population lives in rural areas and is more vulnerable to such causes of death as heart disease, cancer, unintentional injuries, chronic lower respiratory disease, and stroke. They are more vulnerable because they can’t receive necessary medical care due to the lack of medical institutions nearby.
Telehealth can become a key changer in reducing rural deaths due to preventable illness, especially with 5G rushing its way.
Multiple tools and modalities of telehealth are used to improve overall patient care quality. Home monitoring, for example, can be very beneficial for patients recently discharged with a variety of diagnoses. With home monitoring, healthcare providers can track patients’ daily weights, blood pressures, pulse, and oxygen saturation which can indicate when the patient may have a decline in their condition. A study has demonstrated that cardiac patients were less likely to have subsequent emergency room visits and re-hospitalizations after discharge — all thanks to home monitoring tools.
But let’s follow through it step by step without losing the essence.
How it all started

Modern telemedicine, the way we know it today, began in the early 1960s when NASA first put men in space. They measured astronauts’ wellbeing and kept the situation under control via onboard technologies, as well as spacesuits. The results were transmitted to monitoring physicians using satellite technology.
Sometime after, NASA turned its attention back on earth and started a project to deliver healthcare to the Papago Indian Reservation in Arizona. They’ve sent a van with a variety of medical instruments to the isolated population. Two paramedics used the equipment, including an x-ray machine and electrocardiograph, and transmitted the results to specialists via microwave transmission. After that, for many years telemedicine technology was used mostly to connect patients at rural healthcare facilities to specialists in cities.
Thanks to the widespread use of the internet and data transmitting, the use and delivery of telemedicine have become much simpler. The technologies eliminated the need for costly special equipment — like everything else these days, you only need an app.
Telehealth model types
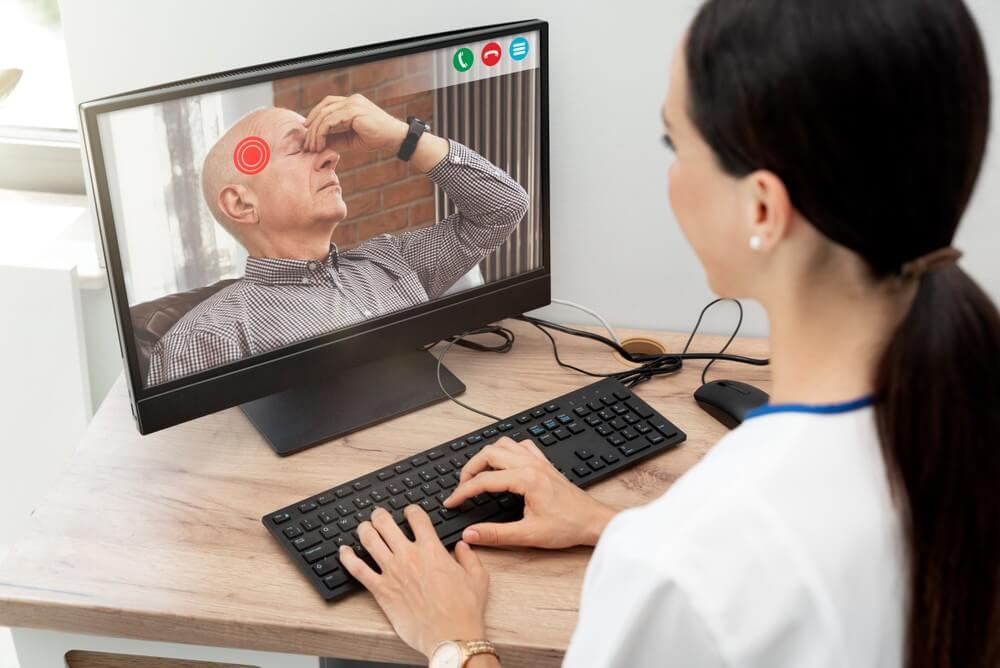
There are a lot of Telehealth models out there, and more are going to come, but the main ones, for now, are Synchronous, Asynchronous, Mobile Health (mHealth), and Hybrid.
- The synchronous model means to deliver health information in real-time through live consultations. This is done, mostly, through interactive video with a patient and physiotherapist present at the same time. It also can be done via chats and cell phones.
- The asynchronous model refers to storing and forwarding, store-and-forward as it commonly called, health information and is used in physiotherapy consultation. Here all the necessary information is being collected at the patient site, then it is assessed and analyzed by a therapist. For example, patients track their activity or steps on a daily basis and it all is transmitted to a physiotherapist for further monitoring and analyses.
- Mobile Health is a mobile-based or mobile-enhanced way of providing medical care. These can be done via phones, tablets, personal digital assistants (PDAs), chatbots, mobile apps, and more. The health-related information here is provided via text messages, recording and transferring relevant data, communicating with providers via video calls, or instant messages. As the mobile world evolves at a tremendously rapid pace, smartphones are becoming ubiquitous, which leads to a vast impact on all aspects of healthcare.
- Hybrid telehealth is where both in-person and telehealth tools cooperate to provide the best service for a patient. Hybrid consultations are most commonly seen in specialties like dermatology and cardiology. It includes a combination of synchronous and asynchronous models and everything that they include: video consultations, home monitoring, telenursing, and a lot more. But first things first.
Telehealth benefits
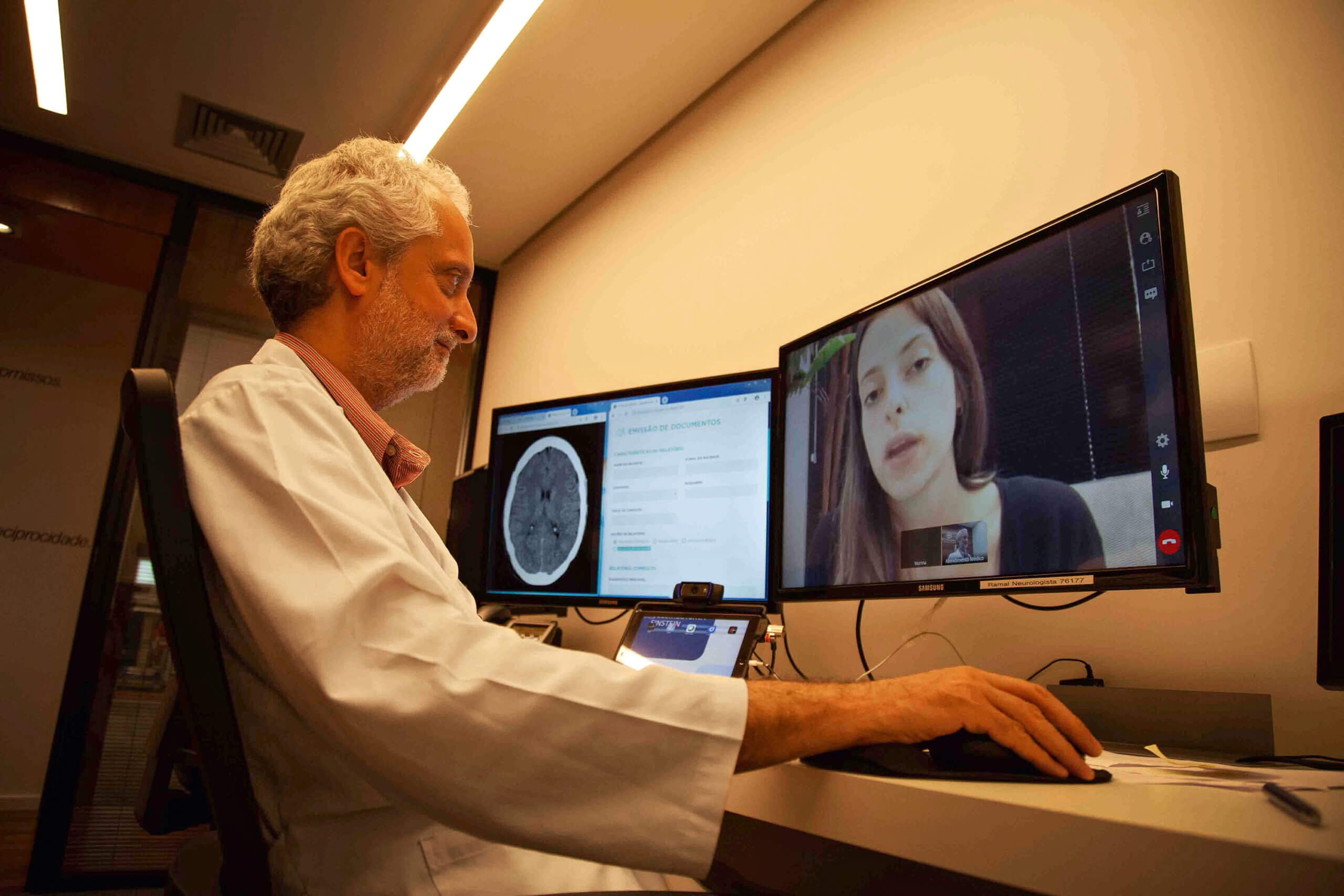
One of the main benefits of Telehealth is that it gives access to medical care at a distance. Patients can receive help in remotely or when physiotherapy is not available in their area. This illuminates such barriers as travel time, parking, and waiting rooms. It is also more flexible for patients as they can schedule therapy at a suitable time.
Remote medical care provided via Telehealth is very beneficial for common situations but becomes even crucial when it comes to some emergency ones.
Like in the case of emergencies in remote environments such as the Antarctic and in ships or airplanes, where it may be difficult, if not impossible, to get medical care to the patient in time.
In countries with unstable or weak economies, where health-care services are often not a priority, telemedicine also grants access to services that would not otherwise be available. Telehealth’s potential could be seen even in the previous century in the case of medical services provision from the city of Arkhangelsk in northwest Russia to other parts of the region and exchange of knowledge and experience between the University Hospital of Tromso, in northern Norway, and northwest Russia.
Reducing, or at least containing, medical costs is another important reason for developing and adopting telehealth technologies. With better management of chronic diseases, shared staffing, reduced travel times, fewer or shorter hospital stays, Telehealth is showing its cost-effective side.
The use of Telehealth shows that the quality of delivered health-care services is as good as that given in traditional in-person consultations. In some specialties, particularly in mental health and ICU care, telemedicine delivers a superior product with greater outcomes and patient satisfaction.
The further the more

This article has been planned as the introductory one. In further articles, you’ll learn about telehealth’s tools in detail and how they can be used to improve our lives as well as telehealth limitations.
The possibilities of telehealth integration into healthcare systems are limitless. The future of Telehealth is widely anticipated among the health care community, especially nowadays. It will be impacting the quality of medical care and patients’ access to care across the continuum.
And if you need assistance with implementing healthcare technology at your hospital and don’t know how to do it right, feel free to schedule an online consultation with our experts. They will answer all your questions about your custom software development needs.









