Computer Vision revamps Teleradiology and Teledermatology
This article is about the benefits and efficiency that Computer Vision brings to image-related parts of healthcare. Since we are digging deep into Telehealth, we’ve picked its two most image-based subspecialties: Teleradiology and Teledermatology.
If you are not familiar with Computer Vision and the way it works — you might be interested in reading our in-depth articles about Computer Vision in sports. If you already know quite a lot about the technology — keep reading further!
For a smooth transition, we’d like to explain Teleradiology and Teledermatology’s story, their basics, and after — the synergy with Computer Vision technology. This way you will have the complete picture. Or you can rush straight to the tech part — it’s up to you.
The story behind
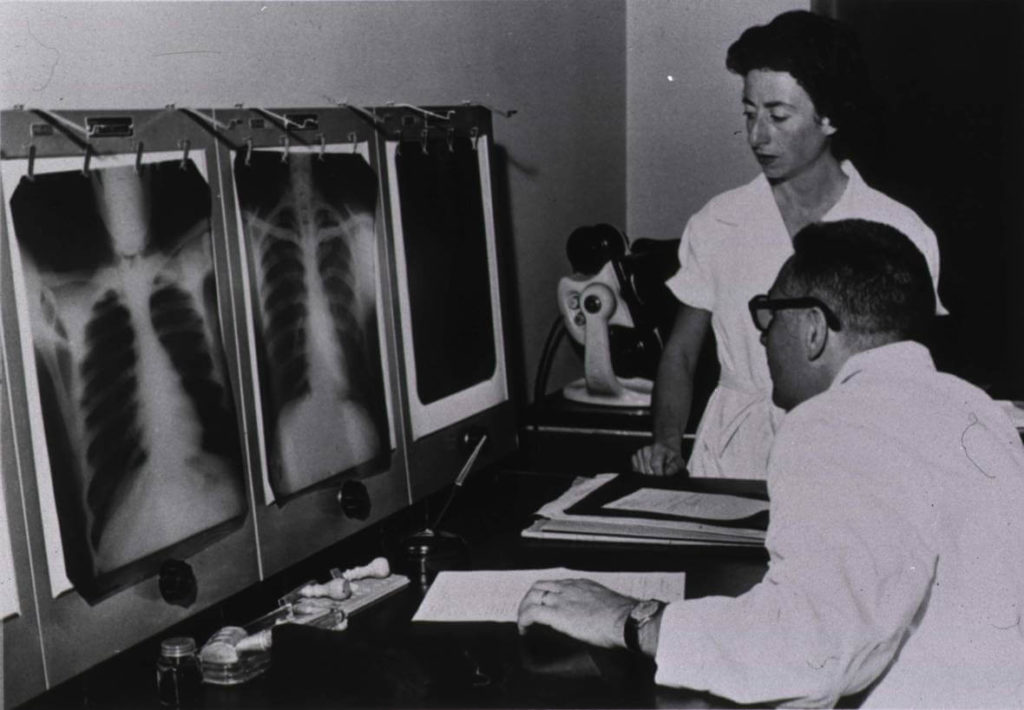
The main idea for Teleradiology technology was the same as for telephone — communication through the use of wire transmissions. This technique was instrumental in telemedicine’s evolution, which is the practice of using doctors that are not in the same place as the patient. Back in 1930, the Queen Mary ocean liner used the marine radiotelephone to receive medical consultation. A doctor on board sent information to external sources for consultations and then served as a consultant for individuals on other ships who needed medical help.
During the 1960s and 1970s, there were extensive experiments and research with transmitting medical images via broadcast television and closed circuits. Images were mostly divided for pathology, dermatology, and radiology needs.
However, the transmission processes were quite tedious, since you could only share one image at a time with quite low-quality resolution and contrast. Due to high maintenance, operational costs, and the experimental nature of such systems, they were more a curiosity versus a practical tool for hospitals.
Soon thereafter, with the Internet and Cloud computing making their appearance, Teleradiology and Teledermatology have flourished into brand-new solutions. Radiologists and dermatologists can now do their work from home and work for several different healthcare companies.
Teleradiology benefits

Since radiology itself is a type of imaging technique (ultrasounds, MRIs, x-rays, etc.) that physicians use for taking images of the internal body parts for either treatment or diagnosis, telecommunications made it possible to perform these techniques remotely. To have a radiologist on-site is quite expensive or, sometimes, impossible. Teleradiology service enables healthcare providers to pay on a per exam basis and for facilities requiring 24/7 services, or the ones with a small volume of radiology patients, it can provide huge savings.
Doctors use teleradiology in order to collaborate and consult with doctors at different locations. It helps with diagnosis and frequently with getting a second opinion, assisting with symptom control. Often it might be even the first opinion since there might not be a radiologist available in a hospital.
Teledermatology models

The idea of Teledermatology is quite similar to Teleradiology — to use telecommunication technologies for transferring medical information over varying distances through audio, visual, and data communication. Teledermatology applications span different areas of health care management like a consultation, diagnoses, treatment, education, and more.
Teledermatology is a subspecialty of Telemedicine, which is part of Telehealth. That means that, like Telehealth and Telemedicine, Teledermatology has the same practice models: Synchronous, or real-time, and Asynchronous, or store-and-forward (SAF). Sometimes SAF and real-time form a Hybrid one.
The SAF model involves sending or forwarding digital images with medical information to a specialist in the field. The main advantages of this method are inexpensive equipment, a mobile phone, for example, and there is no need for both parties to be present at the same time. The real-time model entails medical providers and patients to interact through a live video call. This model is more expensive and requires more expensive technology.
How Computer Vision enhances image analysis and improves Teleradiology
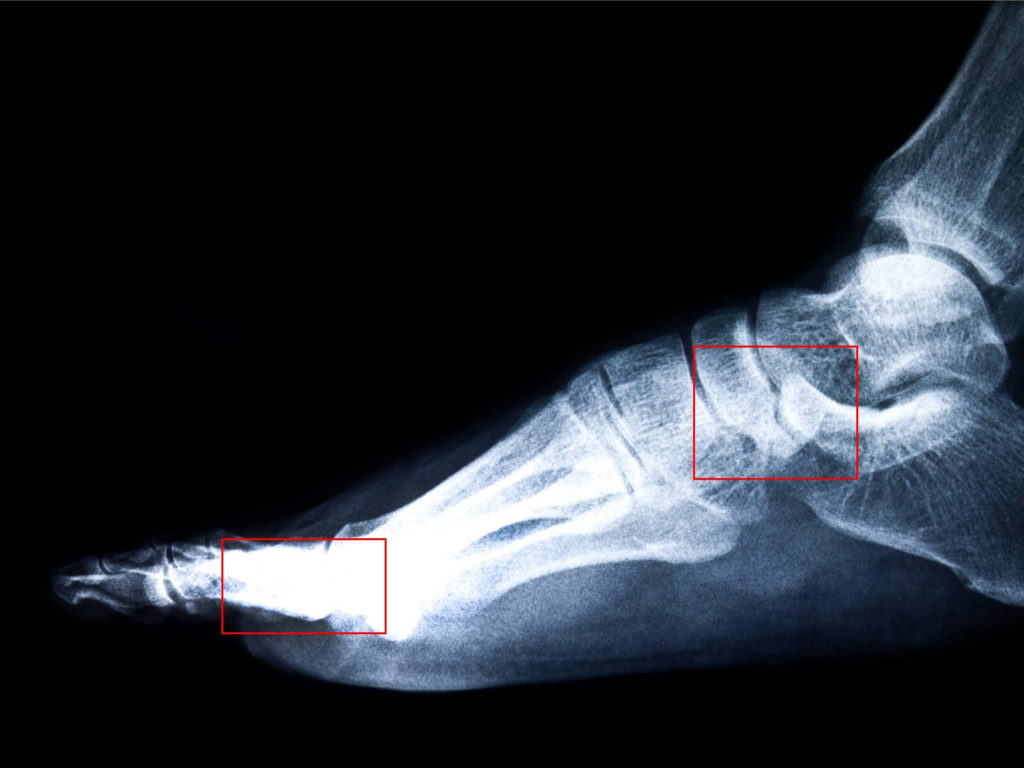
As you can see, Teleradiology and Teledermatology are largely image-based diagnostic specialties and all the generated data is digital or can be converted into a digital format. In each case, specialists need to detect signs of disease, differentiate them from the huge spectrum of normalcy in the human body, perform a multimodal correlation to provide valuable information about the disease, to come up with a diagnosis or a set of diagnostic possibilities. This process involves the tedious task of surfing through thousands of images requiring in-depth attention, as the conclusions about the patient’s problem may be subtle and masked in the deluge of data.
Digital images have a lot more information and embedded data that is beyond human perception. The finely trained Computer Vision algorithms may add an entirely new dimension to image analysis based on quantitative parameters, that is not possible for radiologists and dermatologists.
More efficiency
For example, to quantify tumor treatment initiation and response requires a tedious manual job of segmenting the tumor on each cross-sectional image, which might be hundreds.
But this task can be successfully (and much faster) performed by automated segmentation tools. Computer Vision algorithms can assess various parameters beyond gross anatomical features and, sometimes, indiscernible to the human eye, like shape, pixel density/intensity, texture analysis of a lesion, etc. Unlike the human eye, Computer Vision has no established preferences for data display and can perform without any distortion or details dilution.
Teaching, training, and the skills leveling cycle of specialists sometimes even longer than actual productive years, admitting that detection and interpretation skills remain unequal.
Computer vision algorithms can help radiologists and dermatologists become more accurate by acting as double-checkers, more efficient with accurate detections and quantifications, and more productive as the end result.
More productivity
Computer vision and AI algorithms can help triage cases on the Picture archiving and communication system (PACS) worklist to ensure that the most critical ones get the most immediate attention. By integrating Computer Vision tools into PACS, a preliminary report is generated even before a specialist evaluates a study.
Such a system can prioritize cases based on automated detection, for example, critical cases, such as the head CT with hemorrhage in the brain, are placed at the top and ordinary cases — at the bottom.
Hence, Computer Vision algorithms can build the Smart Segmentation, by acting as lesions finders and formulating a list of differential diagnoses. In the long term, such a system can facilitate complex decision-making by combining interdisciplinary data with visual data to achieve the most reliable diagnosis, recommending further workup and prognosis.
More personalization
Teledermatology can especially benefit from the use of Computer Vision algorithms in hybrid-model systems. For example, users take photos of an annoying lesion through the app, the algorithm categorizes these lesions as low, medium, or high risk and provides treatment recommendations. Users with a high-risk assessment are redirected to a video live-chat with a dermatologist who will review results personally.
Such a system can be trained to detect and categorize any lesion from Solar lentigo and Lipoma to malignant Melanoma.
Even being less accurate, due to the low-quality data, than the eye of a dermatologist, a system can still be effective for users to differentiate benign and malignant lesions.
Another beneficial case for Teledermatology is automated skin analysis for care products recommendation. Computer Vision algorithms analyze camera input, capture facial images, and analyze the main aging areas: forehead, eyes, cheek, mouth, and neck. After a comprehensive analysis, a system identifies problem areas, such as, red spots/blemishes and dark spots, pores, wrinkles, fine lines, dark circles, roughness, and overall skin tone.
This way customers can clearly see the areas that need to be improved and are more likely to be convinced than just simply being advised of using a care product.
In Conclusion
The use of Computer Vision in Teledermatology and Teleradiology has received unprecedented attention from all aspects of the global level, personnel training, scientific research support, technology development, and market capital.
There are still numerous potentials for CV and AI, and more are about to come.
As time goes by, Computer Vision and AI technologies are seeing more and more promotion and innovations, database resources expansions, multi-disciplinary and cross-disciplinary cooperations. This way technology will only bring more professional, accurate, and personalized diagnosis and treatment to healthcare.
In case you have questions about adopting healthcare technology in your organization, feel free to schedule an online consultation with our experts who will gladly assist you with your custom software development needs.